Myoma Symptoms and Treatment Options: What You Need to Know
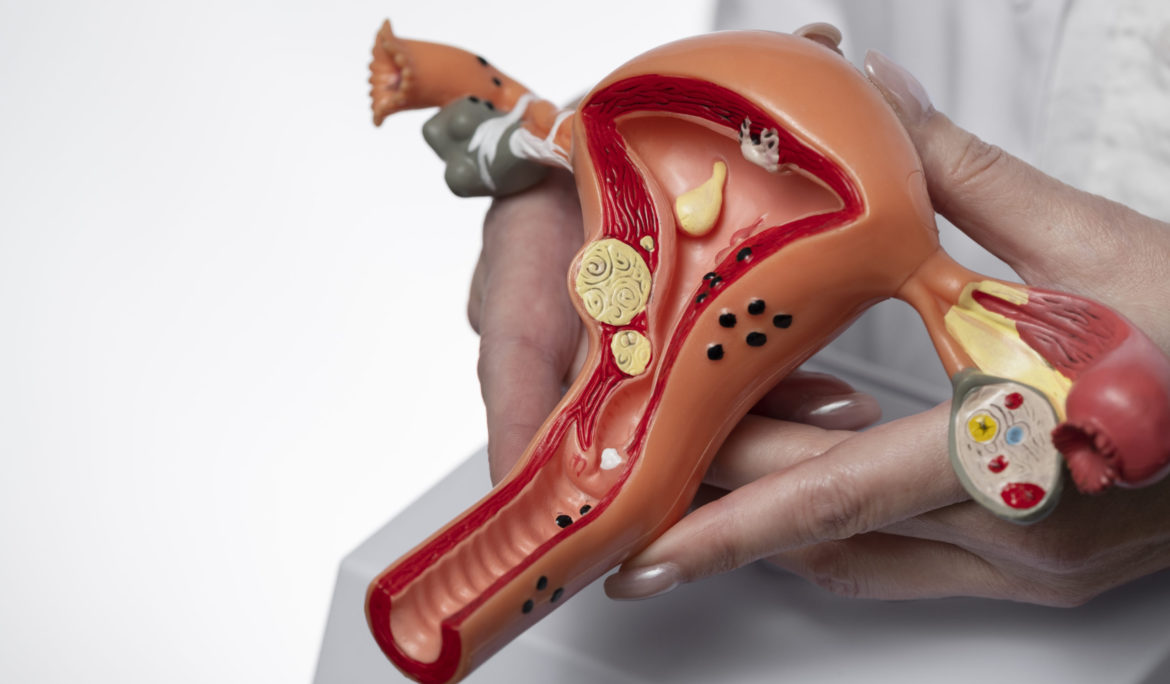
Myomas, more commonly known as uterine fibroids, are non-cancerous growths of the uterus that typically appear during childbearing years. These fibroids are among the most common gynecological conditions, affecting a significant number of women. Despite their prevalence, the exact cause of myomas remains unclear. However, factors like hormones and genetics play a crucial role. This comprehensive guide delves into the symptoms of myomas, their diagnosis, and the various treatment options available, providing essential knowledge for those affected.
Understanding Myoma
Myomas are made from muscle and fibrous tissue and can vary in size. Some are microscopic, whereas others can be large enough to distend the uterus. They may grow as a single tumor or in clusters. Myomas are classified based on their location in the uterus: submucosal (into the uterine cavity), intramural (within the uterine wall), and subserosal (on the outer wall of the uterus).
Symptoms of Myoma
Symptoms of myoma, or uterine fibroids, can vary widely depending on the size, number, and location of the fibroids. Not all women with myomas experience symptoms, but when they do occur, they may include:
- Heavy Menstrual Bleeding: One of the most common symptoms. Periods may be longer than usual and exceptionally heavy, sometimes leading to anemia due to the loss of blood.
- Menstrual Pain and Cramping: Women may experience more severe menstrual cramps than usual.
- Pelvic Pressure or Pain: As fibroids grow, they can cause a feeling of fullness or pressure in the lower abdomen. In some cases, this can progress to persistent or severe pain.
- Frequent Urination or Difficulty Emptying the Bladder: Large fibroids can press against the bladder, leading to frequent urination or difficulty in fully emptying the bladder.
- Constipation: Fibroids that press against the rectum may cause constipation.
- Backache or Leg Pains: Fibroids can exert pressure on nerves in the back and legs, leading to pain in these areas.
- Pain During Intercourse: Depending on the fibroid’s location, some women may experience discomfort or pain during sexual intercourse.
- Complications during Pregnancy and Labor: Myomas can lead to fertility issues, complications during pregnancy, and a higher likelihood of needing a Cesarean section during delivery.
- Swelling or Enlargement of the Abdomen: Large fibroids can cause noticeable swelling or enlargement of the lower abdomen.
It’s important to note that the presence of these symptoms does not definitively indicate myomas, as other medical conditions can cause similar symptoms. Therefore, a proper medical diagnosis is essential for anyone experiencing these symptoms.
Diagnosis of Myoma
The diagnosis of myoma, or uterine fibroids, typically involves a combination of clinical evaluation and imaging studies. The process for diagnosing myomas includes:
-
Medical History and Physical Examination:
- Medical History: The doctor will ask about menstrual cycles, symptoms such as heavy menstrual bleeding and pelvic pain, and any history of uterine fibroids in the family.
- Pelvic Exam: This examination helps the doctor feel for abnormalities in the uterus, ovaries, and other pelvic organs. Myomas might be detected as firm, irregularly shaped lumps in the uterus.
-
Ultrasound:
- The most common initial imaging test used to diagnose myomas.
- It uses sound waves to create images of the uterus and can show the presence, size, and location of fibroids.
- Both abdominal and transvaginal ultrasound might be employed for more detailed imaging.
-
Magnetic Resonance Imaging (MRI):
- An MRI may be used for a more accurate assessment of the number and size of the fibroids, especially when surgery is being considered.
- It provides detailed images of the uterus, ovaries, and other pelvic organs.
-
Hysteroscopy:
- A hysteroscope, a thin, lighted telescope, is inserted into the uterus through the cervix.
- It allows the doctor to examine the inside of the uterus and the endometrium (lining of the uterus) for fibroids protruding into the uterine cavity.
-
Laparoscopy:
- Particularly useful for diagnosing subserosal fibroids (those on the outer surface of the uterus).
- A small camera is inserted into the abdomen through a tiny incision, giving a view of the outside of the uterus.
-
Other Imaging Tests:
- In some cases, a computed tomography (CT) scan may be used, although it’s less commonly employed for fibroid diagnosis.
- Sonohysterography, where fluid is injected into the uterus through the cervix during an ultrasound, may also be used to provide clearer images of the uterine lining and fibroids.
-
Blood Tests:
- While they cannot diagnose fibroids, blood tests can rule out other potential causes of symptoms (like thyroid problems or blood disorders) and check for anemia due to heavy menstrual bleeding.
-
Endometrial Biopsy:
- Although not commonly used for diagnosing fibroids, it can be helpful if there’s a concern about endometrial cancer or other abnormalities.
Each diagnostic tool has its specific role and may be used depending on the individual’s symptoms and medical history. The choice of diagnostic method is often determined by the need for detailed information about the fibroids for treatment planning.
Treatment Options for Myoma
The treatment options for myoma, or uterine fibroids, vary depending on several factors, including the size and location of the fibroids, the severity of symptoms, the woman’s age, her desire to have children, and her general health. Here are the primary treatment options:
-
Watchful Waiting:
- For women with small fibroids that aren’t causing symptoms, or those approaching menopause, watchful waiting is often recommended. Many fibroids shrink after menopause.
-
Medications:
- Hormonal Medications: Birth control pills and other hormonal medications can help control heavy bleeding and painful periods.
- Gonadotropin-Releasing Hormone (GnRH) Agonists: Drugs like leuprolide (Lupron) can temporarily shrink fibroids and stop menstrual periods.
- Progestin-Releasing Intrauterine Device (IUD): Can relieve heavy bleeding caused by fibroids.
-
Non-Invasive Procedure:
- MRI-Guided Focused Ultrasound Surgery (FUS): A non-invasive treatment that uses high-frequency sound waves to heat and destroy fibroid tissue.
-
Minimally Invasive Procedures:
- Uterine Artery Embolization (UAE): Small particles are injected into the uterine arteries, cutting off blood supply to fibroids, and causing them to shrink.
- Laparoscopic or Robotic Myomectomy: Removes fibroids through small incisions in the abdomen, preserving the uterus.
- Endometrial Ablation: Destroys the lining of the uterus to reduce menstrual bleeding, not suitable if future pregnancy is desired.
-
Surgical Procedures:
- Abdominal Myomectomy: Removes fibroids through a larger incision in the lower abdomen. Suitable for large or multiple fibroids.
- Hysterectomy: Surgical removal of the entire uterus, the only permanent solution for fibroids. This procedure is typically considered when other treatments have failed, and the woman does not wish to have children.
-
Lifestyle and Home Remedies:
- Regular Exercise: Can help manage symptoms like pain and maintain a healthy weight.
- Dietary Changes: Eating a balanced diet and maintaining a healthy weight may offer some benefits.
- Over-the-Counter Pain Relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) can be effective in managing pain.
-
Alternative Therapies:
- While not a substitute for traditional treatment, therapies like acupuncture or herbal remedies may offer symptom relief for some women. It’s important to discuss these options with a healthcare provider.
-
Holistic Approaches:
- Stress reduction techniques, yoga, and meditation might help manage symptoms.
The choice of treatment depends on individual circumstances and should be made after thorough discussion with a healthcare provider. For women planning to have children, preserving the uterus and fertility is a key consideration in choosing the appropriate treatment.
Lifestyle and Home Remedies
Alongside medical treatments, lifestyle adjustments can help manage symptoms:
- Regular exercise and a balanced diet.
- Iron supplements to prevent or treat anemia caused by heavy periods.
- Heat therapy, like a warm bath or a heating pad, can alleviate pain.
Conclusion
Understanding the signs and available treatments for myomas is essential for making informed health decisions. Regular health check-ups, open communication with healthcare providers, and a proactive approach to symptoms are key to managing this condition effectively.
FAQs about Myomas (Uterine Fibroids)
What are myomas?
Myomas, also known as uterine fibroids, are non-cancerous growths of the muscle and fibrous tissue on or in the uterus. They vary in size and may appear singly or in clusters.
What causes myomas to develop?
The exact cause is unknown, but factors like hormones (estrogen and progesterone) and genetics play a crucial role in their development.
What are the symptoms of myomas?
Symptoms can include heavy menstrual bleeding, severe menstrual cramps, pelvic pressure or pain, frequent urination, difficulty emptying the bladder, constipation, backache, leg pains, pain during intercourse, complications during pregnancy, and visible swelling of the abdomen.
How are myomas diagnosed?
Diagnosis may involve a pelvic exam, ultrasound, MRI, hysteroscopy, laparoscopy, and sometimes blood tests to rule out other conditions.
What treatment options are available for myomas?
Treatment options range from watchful waiting, medications (hormonal medications, GnRH agonists, progestin-releasing IUD), non-invasive procedures (MRI-guided focused ultrasound surgery), minimally invasive procedures (uterine artery embolization, laparoscopic or robotic myomectomy, endometrial ablation), to surgical procedures (abdominal myomectomy, hysterectomy).
Can myomas affect fertility?
Yes, myomas can lead to fertility issues and complications during pregnancy, including a higher likelihood of needing a Cesarean section.
Do myomas require surgery?
Not always. The need for surgery depends on the size, number, location of the fibroids, severity of symptoms, age, desire to have children, and overall health of the woman.
Can myomas lead to cancer?
Myomas are typically benign and not associated with an increased risk of uterine cancer.
Are there lifestyle or home remedies that can help with myomas?
Yes, regular exercise, a balanced diet, iron supplements for anemia, and heat therapy for pain can help manage symptoms. Stress reduction techniques, yoga, and meditation might also provide relief.
Can myomas recur after treatment?
Yes, myomas can recur, especially if the ovaries are left in place after treatment. Ongoing management and follow-up with a healthcare provider are important.
Feel free to reach out to us with any inquiries regarding myoma or other fertility-related concerns.


